January 18, 2023
Do Insurance Companies Cover Varicose Vein Treatment?
1.3k0
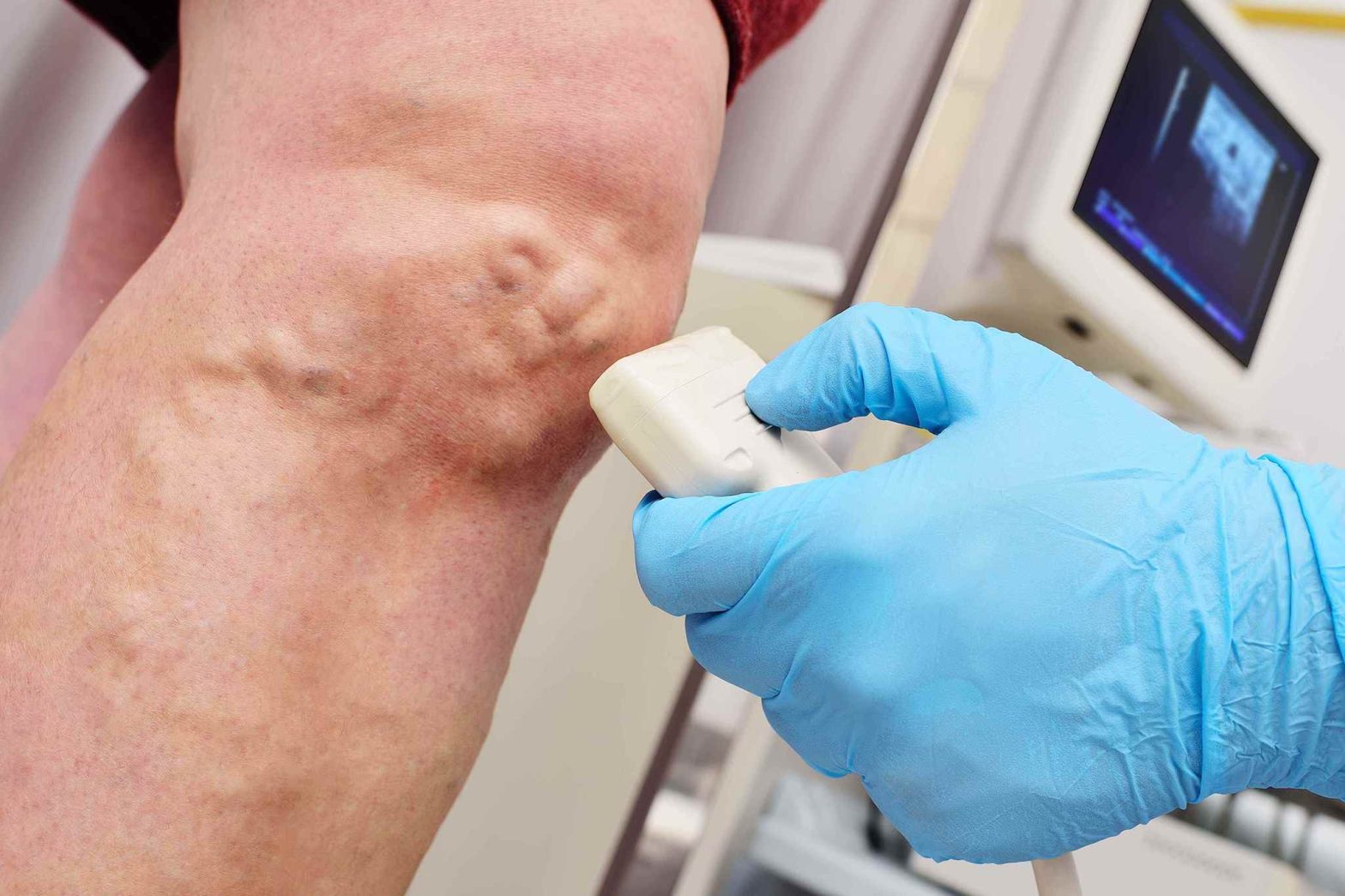
Covering the cost of cosmetic varicose vein treatment?
Vein treatments, whether medical or cosmetic, can aid in removing pronounced or ugly lines. Also, it restores a smoother, more natural-looking complexion. Even though your operation might not be considered medically necessary, it is still worthwhile to pay for. Especially if it gives you more confidence in your appearance. In addition, numerous systems and plans are available to make your vein procedure financially practical for patients worried about the cost of treatment. You might be suitable for a health savings account (HSA), which would let you write off the expenditure of your treatment care when you present your taxes. Alternatively, you might be qualified for a flexible spending account and a benefit offered only by your employer. It might aid in paying for your medical expenses. To guarantee a flawless and easy treatment process, the helpful staff at the vein care center would be pleased to go over financing options with you.What is the medically essential treatment?
If you leave it untreated, some vein diseases can negatively affect health. A treatment required to safeguard or preserve your health, wellness, or general comfort qualifies as medically necessary. For instance, you may be qualified for insurance coverage if you are enduring unpleasant or uncomfortable physical symptoms brought on by varicose veins, such as swelling, tenderness, or heaviness in the affected area. A venous ultrasound can be used to assess whether treatment is medically essential. A quick in-office treatment called a vein screening can reveal your veins' overall health and quality and any hidden issues veins that might endanger your comfort or your health. Your procedure will be considered medically essential. It is reimbursed by insurance if the ultrasound finds signs of edoema, ulceration, or backward blood flow. Most insurers will ask to see your ultrasound results to certify that treatment is necessary for your health.When are vein treatments considered cosmetic?
If the vein treatment addresses the issues and concerns related to your appearance and aesthetic goals, you can consider them cosmetic. Although these methods are not medically essential, they may perform these to address emotional matters like insecurity or self-consciousness. However, because the process is not medically required, it will be viewed as cosmetic and most likely not be compensated by your health insurance company.Conclusion
The above-provided details and information talk about insurance coverage for varicose veins. For more informative updates, please visit veintreatmentnyc.com.RECOMMENDED FOR YOU
Sleeping Habits for Better Autoimmune Recovery
January 2, 2026
What Makes HYROX the Ultimate Fitness Challenge?
October 15, 2025
Are Teeth Implants Affordable Near Me?
October 2, 2025